What are the main treatment goals for sleep apnoea?
The goal is to keep the airway open during sleep, stop breathing interruptions, and normalise oxygen levels. Treatment should also reduce snoring, improve daytime sleepiness, and lower longer-term risks linked with untreated sleep apnoea.
Clinicians usually tailor treatment to the type, obstructive sleep apnoea (OSA) or central sleep apnoea (CSA), plus severity and individual anatomy.
How does CPAP work, and why is it often the first choice?
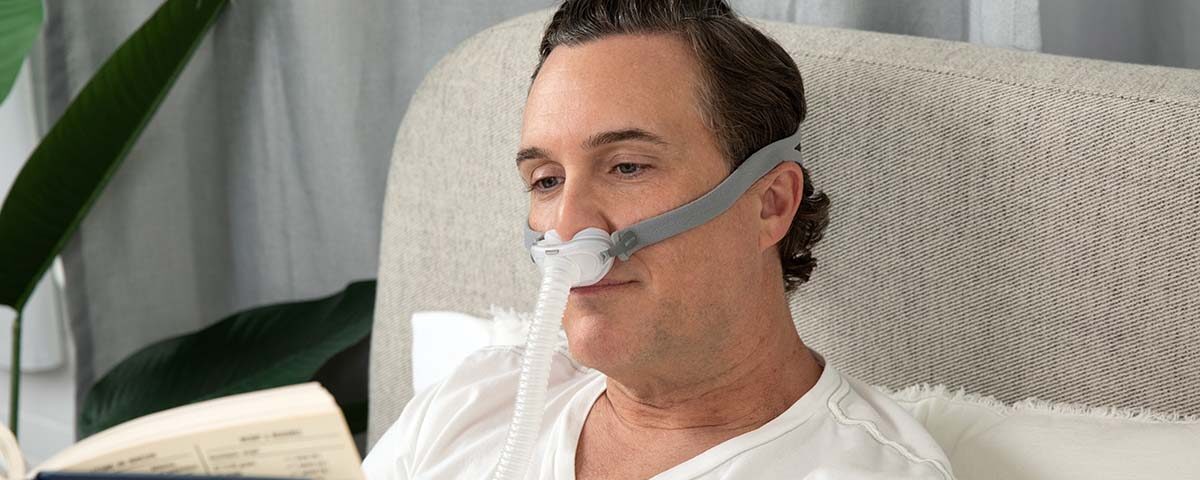
A steady flow of Oxygen air keeps the upper airway open by delivering pressurised air through a mask. It is typically the first-line treatment for moderate to severe OSA because it is highly effective when used consistently. Many people notice improvements in alertness and sleep quality within days to weeks. The main challenge is comfort, which can usually be improved by changing masks, adjusting humidity, or using pressure ramp features.
What is APAP or BiPAP, and when might they be used instead of CPAP?
APAP automatically adjusts pressure throughout the night, which can help people whose pressure needs vary by sleep position or sleep stage. BiPAP provides different pressures for inhalation and exhalation and is often considered when higher pressures are needed or when exhaling against CPAP feels difficult.
These options are commonly used when CPAP is poorly tolerated, or when specific breathing patterns and co-existing conditions make fixed pressure less suitable.
Can oxygen therapy treat sleep apnoea on its own?
Oxygen therapy does not usually treat the airway obstruction that causes OSA, so it is not typically a stand-alone solution. It may improve oxygen levels but still allow repeated breathing pauses, sleep fragmentation, and strain on the cardiovascular system.
Clinicians may prescribe oxygen in selected cases, such as certain forms of CSA, overlap with chronic lung disease, or when oxygen levels remain low despite other treatments. It should be medically supervised, as inappropriate use can worsen carbon dioxide retention in some conditions.
How do mandibular advancement devices help, and who are they best for?
Mandibular advancement devices (MADs) are custom dental appliances that move the lower jaw forward to keep the airway more open. They are often suitable for mild to moderate OSA, or for people who cannot tolerate CPAP.
They can be effective for snoring and may reduce apnoea severity, though results vary. Fit and follow-up matter, as jaw discomfort, bite changes, or tooth movement can occur over time.
What lifestyle changes can meaningfully reduce sleep apnoea severity?
Weight reduction can substantially improve OSA in many people because fat distribution around the neck and tongue can narrow the airway. Avoiding alcohol near bedtime, reducing sedative use where possible, and improving nasal breathing can also reduce collapse risk.
Side sleeping can be helpful for positional OSA, where events worsen on the back. Regular sleep timing and treating nasal congestion can further improve symptoms and tolerance of other therapies.
What is positional therapy, and does it actually work?
Positional therapy aims to keep people off their back during sleep, using wearable devices, pillows, or vibration prompts. It can work well for those whose apnoea is significantly worse when supine.
It is not a complete solution for everyone, especially if events remain frequent in side sleeping. It is often used alongside weight management, nasal care, or PAP therapy.
Which surgical options exist, and when are they considered?
Surgery is typically considered when anatomy is a major contributor, or when non-surgical options are ineffective or intolerable. Options include procedures on the soft palate, tonsils, tongue base, or jaw, depending on where the airway collapses.
Some people benefit from septoplasty or turbinate reduction to improve nasal airflow, mainly to help PAP tolerance. Outcomes vary, so careful assessment and realistic expectations are important.
What is hypoglossal nerve stimulation, and who may qualify?
Hypoglossal nerve stimulation is an implanted device that activates tongue muscles during sleep to reduce airway collapse. It can help selected adults with moderate to severe OSA who cannot use CPAP and meet specific anatomical and body weight criteria.
It is not appropriate for everyone, and it requires surgical implantation and follow-up adjustments. When suitable, it can reduce apnoea events and improve sleep-related quality of life. Learn more about Oxygen Tank vs Oxygen Concentrator for Home Use: Which Should You Choose?
How is central sleep apnoea treated differently from obstructive sleep apnoea?
CSA involves reduced or absent breathing effort rather than a blocked airway, so treatment focuses on stabilising breathing control. Management may include optimising underlying causes such as heart failure, medication effects, altitude-related triggers, or neurological factors.
Some people may be treated with PAP variants designed for central events, and others may require targeted medical management. A clear diagnosis from a sleep study is essential because treatments that help OSA may not address CSA.
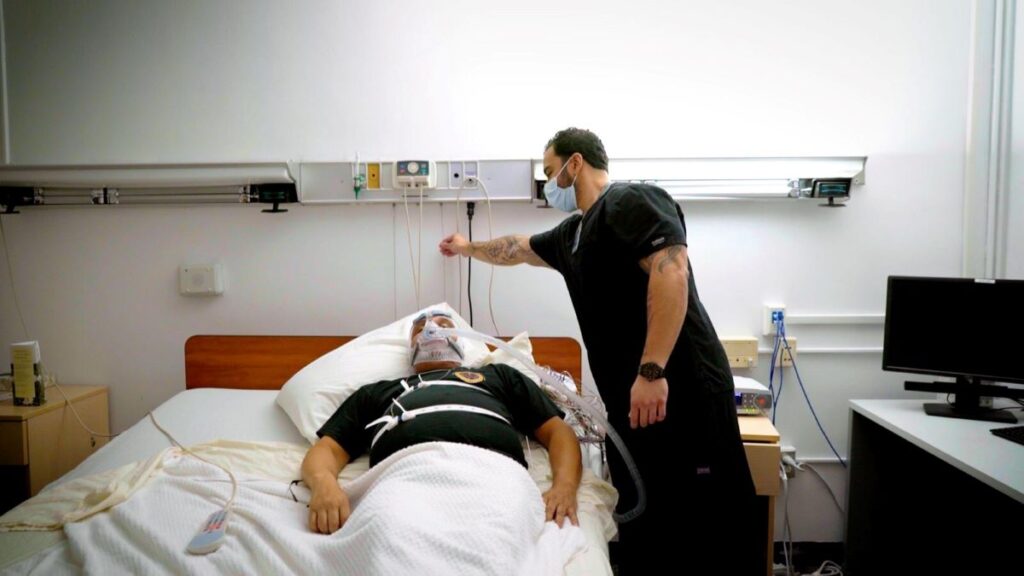
What practical steps improve comfort and long-term success with PAP therapy?
Mask fit is often the biggest factor, so trying different mask types can be transformative. Heated humidification can reduce dryness, and gradual pressure changes can help people adjust, especially early on.
Support matters too. Follow-up with a sleep clinic, checking leak data, and addressing nasal blockage can turn an “intolerable” setup into one that feels routine.
How should they choose the right treatment option?
They should base decisions on a sleep study result, symptom burden, medical history, and personal tolerance. For many, CPAP remains the most reliable option, while MADs, positional therapy, and lifestyle changes can be appropriate for mild to moderate cases or as add-ons.
If symptoms persist, reassessment is important rather than simply “pushing through”. The best plan is usually the one they can actually use consistently, with measurable improvement in sleep quality and breathing events.
FAQs (Frequently Asked Questions)
What are the primary goals of treating sleep apnoea?
The main treatment goals for sleep apnoea are to keep the airway open during sleep, stop breathing interruptions, and normalise oxygen levels. Treatment also aims to reduce snoring, improve daytime sleepiness, and lower long-term health risks associated with untreated sleep apnoea.
How does CPAP therapy work and why is it often recommended first?
CPAP (Continuous Positive Airway Pressure) therapy works by delivering a steady stream of pressurised air through a mask to keep the upper airway open during sleep. It is typically the first-line treatment for moderate to severe obstructive sleep apnoea (OSA) due to its high effectiveness when used consistently, leading to rapid improvements in alertness and sleep quality.
When are APAP or BiPAP machines used instead of CPAP?
APAP (Auto-adjusting Positive Airway Pressure) automatically adjusts pressure throughout the night, suitable for those whose pressure needs vary by sleep position or stage. BiPAP (Bilevel Positive Airway Pressure) provides different pressures for inhalation and exhalation and is often used when higher pressures are needed or when exhaling against CPAP is difficult. These are considered when CPAP is poorly tolerated or specific breathing patterns require variable pressure.
Can mandibular advancement devices effectively treat sleep apnoea?
Mandibular advancement devices (MADs) are custom dental appliances that move the lower jaw forward to keep the airway open. They are effective for mild to moderate OSA or for individuals who cannot tolerate CPAP. While they can reduce snoring and apnoea severity, results vary and proper fit plus regular follow-up are essential to manage potential side effects like jaw discomfort or tooth movement.
What lifestyle changes can help reduce the severity of sleep apnoea?
Meaningful lifestyle changes include weight reduction, which decreases fat around the neck and tongue; avoiding alcohol near bedtime; reducing sedative use; improving nasal breathing; sleeping on one’s side (positional therapy); maintaining regular sleep schedules; and treating nasal congestion. These changes can reduce airway collapse risk and enhance tolerance of other treatments.
How is central sleep apnoea managed differently from obstructive sleep apnoea?
Central sleep apnoea (CSA) involves reduced or absent breathing effort rather than airway blockage seen in obstructive sleep apnoea (OSA). Treatment focuses on stabilising breathing control by addressing underlying causes such as heart failure, medications, altitude effects, or neurological issues. PAP therapies tailored for central events or targeted medical management may be used, emphasising the importance of accurate diagnosis via a sleep study.